
 Interaction with a person suspected of Mpox in Alupe hospital Isolation Center./KNA
Interaction with a person suspected of Mpox in Alupe hospital Isolation Center./KNA
At the border where Kenya meets Uganda lies Busia County, a strategic gateway and a public health pressure point.
With an estimated 1,800 people crossing daily through the Busia and Malaba border points, the county has found itself repeatedly on the frontline of outbreaks from COVID-19 to cholera and now Mpox.
In the year 2020-2023, the county recorded a total of 6418 cases of Covid 19. This was followed by an outbreak of measles in November 2021, where the county recorded 4 cases.
In July, 2023 there was an outbreak of cholera, where a total of 17 cases were recorded. The county was faced by yet another outbreak of Mpox in 2024 in which so far, 59 cases have been recorded with two fatalities of persons who had other underlying health conditions.
Busia County Chief Officer for Public Health and Sanitation Susan Outa says the county is mainly affected whenever there is an outbreak due to the fact of being a gateway county.
This exposes the county to higher risk and this makes their surveillance systems to be always active.
“When Mpox cases were first reported in the region, we moved quickly, relying on lessons from past outbreaks. Alupe Sub-County Hospital was designated as the Mpox isolation center due to its unique location and infrastructure,” said the chief officer.
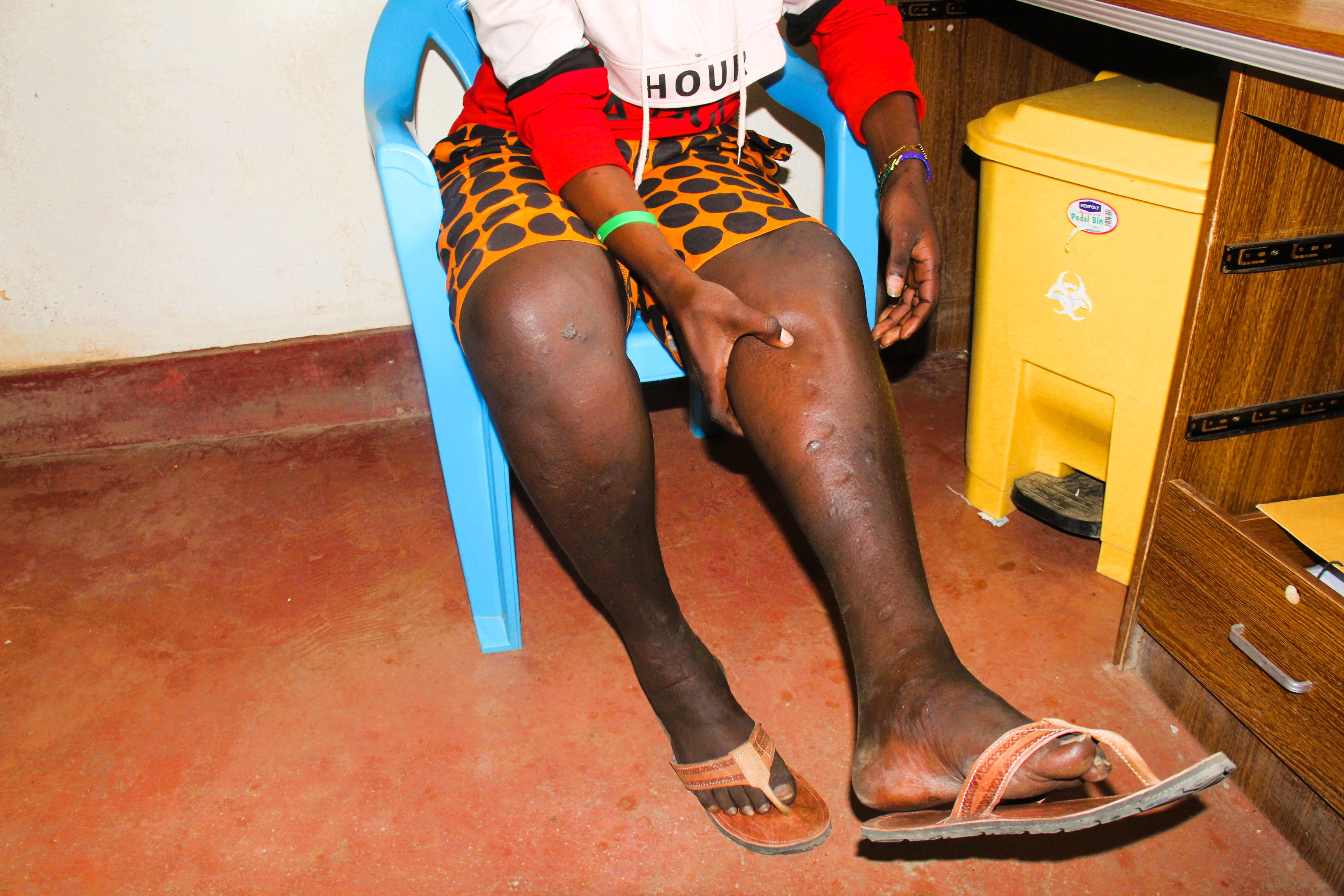 Peter Gakuru showing us his swollen legs and the scars left after recovering from Mpox./KNA
Peter Gakuru showing us his swollen legs and the scars left after recovering from Mpox./KNA
“There’s still a stigma associated with Alupe hospital. It was the COVID-19 isolation center, and now with Mpox, people fear coming here for general health services,” she explains.
To tackle this, the county has launched public sensitization campaigns, reopening Alupe sub county hospital to general patients and encouraging trust in the facility once again.
Outa says the county is now promoting home-based care for stable Mpox patients to reduce congestion at isolation facilities and lessen the stigma.
“We have proposed the creation of a dedicated, stand-alone isolation center to ensure that patients can be treated without compromising the use of other facilities. We’ve submitted a proposal and allocated Sh2 million in our budget for Mpox response. But we also need more,” Outa notes.
Through the partnership of the national government, Red-Cross and UNICEF, provision of critical support in staff training, public education and stakeholder’s sensitisation has been enabled thereby improving the preparedness of the county’s response.
Religious leaders, sex workers, truck drivers, and local administration officers have all been engaged in awareness campaigns
“Our hope is to establish an emergency response fund at the county level, so we’re not always waiting for national intervention when outbreaks occur," Outa said.
"A dedicated surveillance vehicle has also been deployed, enabling real-time contact tracing and monitoring of suspected cases across the county, a crucial step in breaking transmission chains."
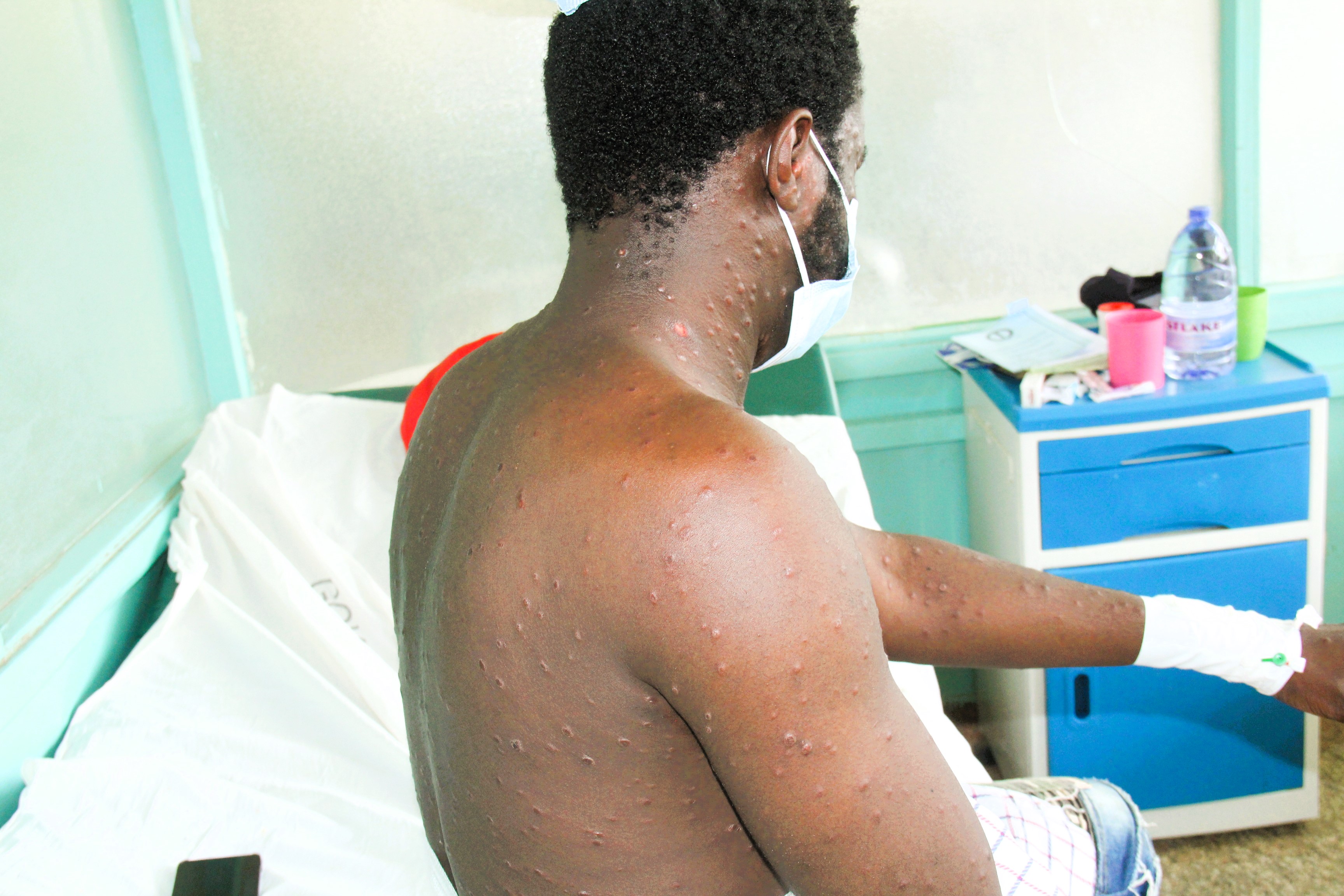 Kevin Fredrick showing us the signs of Mpox on his body at Alupe sub county hospital isolation center as he waits for the results of his samples./KNA
Kevin Fredrick showing us the signs of Mpox on his body at Alupe sub county hospital isolation center as he waits for the results of his samples./KNA
Busia’s leadership has also extended across borders. In collaboration with Ugandan counterparts, the county has held ‘One Health’ forums to discuss early warning systems, cross-border case handling, and community-level signal detection.
“We contained a cholera outbreak in 2023. We can handle Mpox too but it takes preparation, partnerships, and policy,” says confident Outa.
In 2020, as the world grappled with COVID-19, Busia County took decisive steps to strengthen its preparedness for health emergencies.
At the heart of this effort was the Emergency Operations Centre (EOC), launched to manage the county’s response to outbreaks, a critical lifeline given that Busia has several porous borders and heavy cross-border traffic.
According to the Centre Manager Jude Oduor, the EOC was set up to ensure quick and effective response. It works closely with multiple stakeholders, including immigration, health officials, and security agencies to screen travelers entering Kenya. Suspected cases are quarantined immediately to prevent community spread.
“During the COVID-19 pandemic, we managed 6,418 cases in Busia alone. Today, the focus has shifted to Mpox, in which EOC has managed 59 cases as of August 1st, 2025, coordinating contact tracing, isolation, and public information efforts,” says Oduor.
The manager says samples from suspected Mpox patients are taken at the Busia County Referral Hospital laboratory.
For accuracy and reliability, two samples are collected, one tested locally, and the other sent to the national government laboratory for confirmation and cross-verification.
“This dual-testing approach helps ensure we don’t miss any cases and maintain trust in our diagnosis. It also strengthens collaboration between county and national health systems, enabling timely interventions,” Oduor says.
 Busia County Referral Hospital Laboratory Linet Munyasa (R) describing to the Busia county chief for public health and sanitation Susan Outa how the machines at the lab work./KNA
Busia County Referral Hospital Laboratory Linet Munyasa (R) describing to the Busia county chief for public health and sanitation Susan Outa how the machines at the lab work./KNA
PANIC AND PAIN
According to Jane Achodo, the nurse in charge, when the first case of Mpox arrived at Alupe sub-county hospital in July 2024, panic rippled through the wards
The memories of COVID-19 were still raw, and for health workers on the ground, this new virus brought back feelings of discomfort.
“We weren’t well sensitised when the first Mpox case came in,” recalls Achodo, “It was a horrible moment for many of us. We feared the unknown, especially since Mpox, like COVID, doesn’t have a specific drug.”
She further explained that the fear didn’t last. Rapid sensitization efforts by the county and national government equipped the staff with knowledge and confidence.
Drawing on their COVID-19 experience, the team at Alupe sub county hospital quickly adapted, reusing protocols, isolation procedures, and personal protective equipment (PPE) that had once protected them during the height of the Covid pandemic.
“We realised Mpox and COVID-19 had a lot of similarities in how we handle them, so we applied the same approach and used supportive drugs from our facility to manage symptoms and prevent complications,” she said.
Achodo stated that of the 59 confirmed Mpox cases in Busia, two patients sadly died both with underlying health conditions.
“For many patients with mild symptoms, home-based care remains the preferred option. But that, too, comes with risk. We are constantly advising those recovering at home to avoid body contact and follow isolation guidelines strictly,” Achodo added.
She said the persistent battle for the facility is that of fighting stigma. Despite being reopened to the public, Alupe Hospital still carries the weight of public fear.
“People are not coming back for regular services,” she admits. “Even though we offer quality care, the stigma from COVID and now Mpox has kept people away. Staffing is another concern. The team at Alupe hospital needs more health workers to be deployed to the facility for it to be in a better position to handle all situations,” nurse Achodo observed.
Inside one of the rooms at Alupe sub county hospital’s Mpox isolation center, Kevin Fredrick sits calmly, his body bearing signs of a disease that has been witnessed in Busia.
He is not yet confirmed positive for Mpox as his test results are pending but the symptoms are consistent.
“It started with some itching and then boil-like things started showing on my body,” Kevin, a cyber operator and graphic designer in Busia town says. Initially he thought it was a mild skin allergy and went to Busia County Referral Hospital, where he was treated for an allergic reaction and sent home.
“When I got home, it kept getting worse. That’s when I decided to come here on my own. Health workers who are experienced from prior cases, quickly recognized the warning signs and advised that I stay in isolation while awaiting test results,” he explains.
Despite the unfamiliar surroundings, Kevin appears composed. He says the care he has received from the nurses has made the experience less frightening.
“Yes, it was strange and unexpected. I don’t know how I got it, maybe at work but no one else around me has shown any symptoms. What’s helping me is the way the nurses talk to me. I’m psychologically prepared for any result and with the way I’m being treated here, I believe I’ll leave soon,” he says with optimism.
GET HELP WHEN YOU FELL UNUSUAL
In his message to the public, Kevin says, “If you feel anything unusual don’t wait. Go to a hospital and get help. This place may not be where you’d wish to be, but it’s where you should come to if you suspect anything”.
One Peter Gakuru, a salonist based in Malaba, thought he had just overworked. “After finishing work one day, I felt very weak. I took painkillers and went to bed, thinking I’d be fine in the morning,” he recalls.
He continued to narrate that the next day brought something far more serious. He couldn’t get out of bed, he felt pain at his back, had a headache, and general body weakness.
He sought help at Kocholia sub county Hospital, where he was admitted. For three weeks, doctors monitored his condition, unsure what exactly they were dealing with, then the rash appeared.
“It started on my face. They moved me to another room. After four days, the rash had spread all over my body, and that’s when they suspected Mpox. A sample was taken for testing and came back positive,” he says.
He was immediately transferred to Alupe Hospital, where he spent an additional six weeks in isolation. The journey wasn’t easy, and while the virus eventually left his system, its impact stayed with him.
“When I finally went back home, the place where the sample was taken started to itch. I went back to Kocholia sub county hospital and they found there was a problem under the skin and they had to do surgery,” Peter explains.
Even now, months after discharge, Peter continues to recover. The rashes and visible scars are slowly disappearing, but one major issue remains, his leg is still swollen, a painful reminder of the ordeal.
In another quiet corner of Malaba town, a 64-year-old mechanic from Teso North, shares a similar yet simpler story.
His Mpox symptoms began with small pimple-like spots. Unsure of what it was, he asked his family for advice. They urged him to go to the hospital.
“I had heard about Mpox but had never seen it in anyone,” Geoffrey says. At Kocholia Hospital, a sample taken for testing confirmed he was positive. He was isolated for a week, treated, and then discharged.
“The nurses took care of me. I recovered in a week’s time. Now I’m feeling strong. My family supported me throughout. When you feel sick, don’t wait. Go to the hospital and get help,” he says with a smile.
In Busia County Referral Hospital Laboratory, a quiet but critical war is being fought, one that few outside the health system get to see.
This is where the Lab Manager Linet Munyasa leads a team of experts testing for viral threats like Mpox, HIV, Hepatitis B and C, and HPV.
And while Busia is known for its vulnerability due to high border traffic, it’s also leading in Mpox detection simply because it can test.
“We’re recording higher numbers not necessarily because we have more cases but because we have the capacity to confirm them,” Munyasa explains.
IT A BIG FIGHT
That capacity comes from technology. The lab houses advanced molecular testing machines, including the Alinity M system, which can process up to 300 samples per hour, and the mini-PCR machine, capable of handling 48 samples hourly.
These allow for fast, reliable results across a range of diseases including Mpox.
“So far, the lab has tested 79 suspected Mpox cases, confirming 59 positives and this shows that the virus is present in the community,” said Munyasa.
She admitted that the main challenge was inadequate reagents but indicated that the national government has stepped in, ensuring that the lab remains operational through steady support.
The laboratory doesn’t just serve Busia but also covers Vihiga County, making it a regional diagnostics hub. In outbreak response, time is everything, and Busia’s ability to test locally has likely saved lives by enabling faster isolation and treatment.
In Busia County, the fight against Mpox is more than a public health response; it is a story of people, preparedness, and perseverance.
From the border checkpoints of Busia and Malaba to the corridors of Alupe sub county Hospital, and inside the labs of the referral hospital, the county has mobilized a full-spectrum response: surveillance, testing, isolation, treatment, and human connection.
It has not been easy. Health workers are still bearing the emotional weight and fear of the COVID-19 pandemic and now mpox. Patients like Peter Gakuru battled not only the virus but also its painful aftermath.
Yet, amid these challenges, Busia has stepped up. With support from national agencies, partners like UNICEF and Red Cross, and regional collaboration with Ugandan health officials, the county has created a response model. Laboratories are functioning, communities are being sensitized, and survivors are finding their voice urging others not to wait but to seek help early.
The county continues to advocate for more funding, more health workers, and the establishment of a dedicated emergency response fund.
It is also working to reduce the stigma that keeps residents away from crucial facilities like Alupe sub- county hospital.













